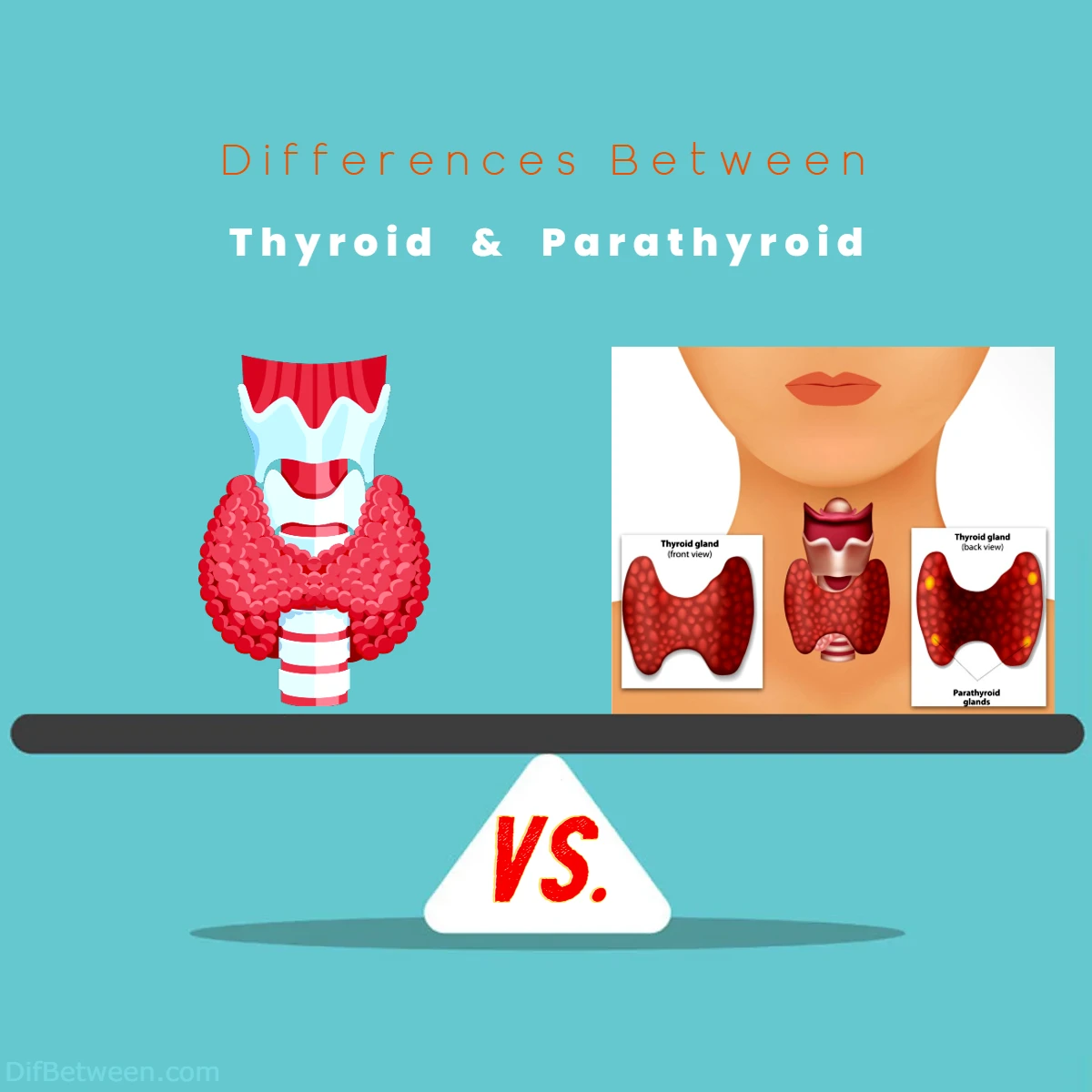
The primary differences between the Thyroid and Parathyroid glands lie in their functions and location. The Thyroid, a butterfly-shaped gland situated in the neck, regulates metabolism and body temperature, producing hormones like T3 and T4. On the other hand, the Parathyroid glands, four small structures located on the posterior surface of the thyroid, primarily control blood calcium levels through the secretion of Parathyroid Hormone (PTH). While the Thyroid directly influences metabolism, the Parathyroid glands play a pivotal role in calcium balance. Understanding these distinctions is crucial for recognizing the unique contributions of these glands to our overall health.
| Characteristic | Thyroid Gland | Parathyroid Glands |
|---|---|---|
| Location | Front of the neck, below the Adam’s apple | Posterior surface of the thyroid gland |
| Number of Glands | Single, butterfly-shaped gland with two lobes | Four separate glands (two upper, two lower) |
| Size | 25 to 35 grams | Rice-sized (small) |
| Primary Hormones Produced | Thyroxine (T4), Triiodothyronine (T3), Calcitonin (minor role) | Parathyroid Hormone (PTH) |
| Function | Regulation of metabolic rate, body temperature, and energy balance | Regulation of blood calcium levels |
| Impact on Metabolism | Directly affects metabolic rate and energy expenditure | Does not have a direct impact on metabolism |
| Hormone Regulation | Controlled by feedback loop involving hypothalamus, pituitary gland, and thyroid hormones | Regulated by blood calcium levels |
| Development and Structure | Develops from the floor of the embryonic pharynx, two lobes connected by isthmus | Develop from the same tissue as the thyroid but migrate to posterior surface of the thyroid |
| Blood Supply | Supplied by superior and inferior thyroid arteries | Supplied by branches of the superior thyroid artery, inferior thyroid artery, and recurrent laryngeal artery |
| Disorders Impacting Calcium Levels | Can indirectly impact calcium levels through bone turnover and medication side effects | Directly involved in calcium regulation, disorders can lead to hypercalcemia (elevated blood calcium) or hypocalcemia (low blood calcium) |
| Surgical Considerations | Thyroidectomy may be performed for thyroid disorders, requiring lifelong hormone replacement therapy | Surgery performed for hyperparathyroidism to remove overactive glands while preserving normal functioning glands |
The thyroid gland, nestled gracefully in the front of your neck, is like the body’s personal thermostat, orchestrating your metabolism, temperature regulation, and energy expenditure. In contrast, the parathyroid glands, four tiny but essential companions, reside on the back of the thyroid and focus their efforts on maintaining the delicate balance of calcium in your bloodstream.
Differences Between Thyroid and Parathyroid
Anatomy and Location
Thyroid Gland
The thyroid gland is a butterfly-shaped endocrine gland situated in the front of the neck, just below the Adam’s apple. It consists of two lobes connected by a narrow band of tissue called the isthmus. This gland, weighing a mere 25 to 35 grams, may be small in size, but it plays a significant role in the body’s overall function.
Thyroid Gland Anatomy
| Characteristics | Details |
|---|---|
| Shape | Butterfly-shaped |
| Location | Front of the neck, below the Adam’s apple |
| Lobes | Two lobes connected by an isthmus |
| Weight | 25 to 35 grams |

Parathyroid Glands
In contrast to the thyroid, the parathyroid glands are not just one, but four small, rice-sized glands located on the posterior surface of the thyroid gland. They are typically found in pairs, with two upper and two lower glands. These glands are essential for calcium homeostasis in the body.
Parathyroid Glands Anatomy
| Characteristics | Details |
|---|---|
| Number | Four glands (two upper, two lower) |
| Location | Posterior surface of the thyroid gland |
| Size | Rice-sized (small) |

Function
Thyroid Gland
The thyroid gland’s primary function is to produce and release thyroid hormones, namely thyroxine (T4) and triiodothyronine (T3). These hormones are crucial for regulating the body’s metabolic rate, which affects how quickly the body uses energy and controls various processes such as temperature regulation and weight management. The thyroid gland responds to signals from the pituitary gland to maintain hormonal balance and ensure the body functions optimally.
In essence, the thyroid gland acts as the body’s thermostat, making sure that your metabolism runs at the right pace, neither too fast nor too slow. It accomplishes this by regulating the levels of T3 and T4 in the bloodstream.
Parathyroid Glands
The parathyroid glands, on the other hand, are responsible for controlling calcium levels in the body. They secrete parathyroid hormone (PTH), which plays a pivotal role in maintaining calcium balance. PTH stimulates the release of calcium from the bones, enhances the absorption of calcium in the intestines, and reduces the excretion of calcium in the urine. All of these actions are aimed at ensuring that the concentration of calcium in the blood remains within a narrow, normal range.
In simple terms, the parathyroid glands act as the body’s calcium regulators, preventing calcium levels from going too low, which could lead to muscle cramps, tingling sensations, or even seizures.
Regulation
Thyroid Gland
The thyroid gland’s activity is regulated by a feedback loop involving the hypothalamus, the pituitary gland, and the thyroid itself. The hypothalamus releases thyrotropin-releasing hormone (TRH), which stimulates the pituitary gland to produce thyroid-stimulating hormone (TSH). TSH, in turn, stimulates the thyroid gland to release T3 and T4. When the levels of T3 and T4 in the blood are sufficient, they signal the hypothalamus and pituitary gland to reduce TRH and TSH production, thus maintaining hormonal balance.
Parathyroid Glands
The parathyroid glands’ activity is primarily controlled by the concentration of calcium in the blood. When blood calcium levels drop, the parathyroid glands release parathyroid hormone (PTH) to increase calcium levels. PTH accomplishes this by promoting calcium release from the bones, enhancing calcium absorption in the intestines, and reducing calcium excretion in the urine. When blood calcium levels are restored to the normal range, PTH secretion decreases.
Common Disorders
Thyroid Gland Disorders
The thyroid gland can be affected by various disorders, some of which are:
Hypothyroidism
Hypothyroidism is a condition in which the thyroid gland doesn’t produce enough thyroid hormones. This can result in symptoms such as fatigue, weight gain, cold intolerance, and depression. The most common cause of hypothyroidism is an autoimmune condition called Hashimoto’s thyroiditis.
Hyperthyroidism
Hyperthyroidism, on the other hand, is characterized by excessive production of thyroid hormones. This condition can lead to symptoms like rapid heart rate, weight loss, anxiety, and tremors. Graves’ disease is a common cause of hyperthyroidism.
Goiter
A goiter is an enlargement of the thyroid gland. It can occur in both hypo- and hyperthyroidism and is often caused by iodine deficiency or autoimmune disorders.
Parathyroid Gland Disorders
The parathyroid glands can also be affected by various disorders, including:
Hyperparathyroidism
Hyperparathyroidism occurs when the parathyroid glands produce too much parathyroid hormone. This leads to elevated levels of calcium in the blood, potentially causing kidney stones, bone pain, and digestive issues. The most common cause of hyperparathyroidism is a non-cancerous tumor in one of the parathyroid glands.
Hypoparathyroidism
Hypoparathyroidism is the opposite of hyperparathyroidism, where the parathyroid glands produce insufficient parathyroid hormone. This results in low levels of calcium in the blood, leading to muscle cramps, seizures, and tingling sensations.
Diagnosis and Treatment
Thyroid Gland Diagnosis and Treatment
Diagnosing thyroid disorders typically involves blood tests to measure TSH, T3, and T4 levels. An ultrasound may also be used to assess the size and structure of the thyroid gland. Treatment for hypothyroidism usually involves hormone replacement therapy with synthetic T4. Hyperthyroidism can be treated with medications that reduce thyroid hormone production or with radioactive iodine therapy. In some cases, surgery to remove part or all of the thyroid gland may be necessary.
Parathyroid Gland Diagnosis and Treatment
Diagnosing parathyroid disorders includes measuring blood calcium and PTH levels. Imaging studies like ultrasound, CT scans, or sestamibi scans may be used to locate abnormal parathyroid glands. Treatment for hyperparathyroidism typically involves surgical removal of the affected gland(s). Hypoparathyroidism is managed with calcium and vitamin D supplements.
Hormones Produced
Thyroid Gland
The primary hormones produced by the thyroid gland are thyroxine (T4) and triiodothyronine (T3). These hormones contain iodine and are responsible for regulating the body’s metabolic rate, affecting how quickly the body uses energy. They influence various bodily functions, including heart rate, temperature regulation, and the rate at which you burn calories. Additionally, the thyroid gland also produces a hormone called calcitonin, which helps regulate calcium levels in the body, although its role is relatively minor compared to the parathyroid glands.
Parathyroid Glands
The parathyroid glands produce a single hormone, parathyroid hormone (PTH), which is primarily responsible for maintaining calcium homeostasis. PTH acts to increase the concentration of calcium in the bloodstream by promoting its release from the bones, enhancing calcium absorption in the intestines, and reducing calcium excretion in the urine.
Role in Calcium Regulation
Thyroid Gland
While the thyroid gland does play a role in calcium regulation through the production of calcitonin, this role is relatively minor compared to the parathyroid glands. Calcitonin helps to lower blood calcium levels by inhibiting the release of calcium from the bones. However, in most cases of calcium balance, the primary responsibility lies with the parathyroid glands.
Parathyroid Glands
The parathyroid glands are the key regulators of calcium balance in the body. They monitor blood calcium levels closely and, when these levels drop, they release parathyroid hormone (PTH) to ensure that calcium is restored to the normal range. PTH acts on the bones to stimulate the release of calcium, on the intestines to increase calcium absorption, and on the kidneys to reduce calcium excretion.
Impact on Metabolism
Thyroid Gland
The thyroid gland has a significant impact on metabolism. It regulates the metabolic rate, which is the rate at which the body converts food into energy. When thyroid hormone levels are too low (hypothyroidism), the metabolic rate slows down, leading to symptoms like fatigue, weight gain, and cold intolerance. Conversely, when thyroid hormone levels are too high (hyperthyroidism), the metabolic rate speeds up, resulting in symptoms such as weight loss, rapid heart rate, and heat intolerance.
Parathyroid Glands
The parathyroid glands do not have a direct impact on metabolism. Their primary function is to regulate calcium levels in the body. Changes in calcium levels can affect muscle function and nerve transmission, but they do not influence the overall metabolic rate as the thyroid gland does.
Hormone Regulation
Thyroid Gland
The production and release of thyroid hormones are regulated by a feedback loop involving the hypothalamus and the pituitary gland. When the levels of thyroid hormones in the blood are too low, the hypothalamus releases thyrotropin-releasing hormone (TRH), which stimulates the pituitary gland to produce thyroid-stimulating hormone (TSH). TSH then prompts the thyroid gland to produce more T3 and T4. When the levels of T3 and T4 are sufficient, they signal the hypothalamus and pituitary gland to reduce TRH and TSH production, maintaining hormonal balance.
Parathyroid Glands
The parathyroid glands’ hormone production is primarily controlled by the concentration of calcium in the blood. When blood calcium levels drop, the parathyroid glands release parathyroid hormone (PTH) to increase calcium levels. Conversely, when blood calcium levels are too high, PTH secretion decreases. This system allows for the precise regulation of calcium levels in the body.
Development and Structure
Thyroid Gland
The thyroid gland originates from the floor of the embryonic pharynx and descends to its final location in the front of the neck during fetal development. It has two lobes connected by a narrow isthmus, giving it a butterfly-like shape. The thyroid is composed of follicles that store and secrete thyroid hormones, and these follicles are made up of epithelial cells.
Parathyroid Glands
The parathyroid glands, on the other hand, develop from the same tissue that gives rise to the thyroid, but they migrate to the posterior surface of the thyroid during embryonic development. They are usually found in pairs, with two upper and two lower glands. Each parathyroid gland consists of chief cells that produce parathyroid hormone (PTH) and oxyphil cells of unknown function.
Blood Supply
Thyroid Gland
The thyroid gland receives its blood supply from the superior and inferior thyroid arteries. These arteries provide the necessary oxygen and nutrients for the production of thyroid hormones and other thyroid functions.
Parathyroid Glands
The blood supply to the parathyroid glands comes from branches of the superior thyroid artery, the inferior thyroid artery, and the recurrent laryngeal artery. These arteries ensure that the parathyroid glands receive adequate blood flow to maintain their function in calcium regulation.
Disorders Impacting Calcium Levels
Thyroid Gland Disorders
Thyroid disorders, particularly hyperthyroidism, can indirectly impact calcium levels. When there is an excess of thyroid hormones, it can lead to increased bone turnover and bone loss, which may affect calcium balance. Additionally, some medications used to treat hyperthyroidism can interfere with calcium absorption, contributing to potential calcium-related issues.
Parathyroid Gland Disorders
Disorders of the parathyroid glands have a direct and significant impact on calcium levels. Hyperparathyroidism, characterized by excess parathyroid hormone, elevates blood calcium levels, potentially leading to symptoms like kidney stones and bone pain. In contrast, hypoparathyroidism, where there is insufficient parathyroid hormone, results in low blood calcium levels, causing muscle cramps and tingling sensations.
Surgical Considerations
Thyroid Gland Surgery
Surgery involving the thyroid gland is typically performed to treat thyroid disorders such as thyroid cancer or large goiters. Thyroidectomy, the surgical removal of part or all of the thyroid gland, may be required. If the entire thyroid gland is removed, the patient will need lifelong hormone replacement therapy to maintain thyroid hormone levels.
Parathyroid Gland Surgery
Surgery related to the parathyroid glands is mainly performed to treat hyperparathyroidism when one or more parathyroid glands become overactive. The goal is to remove the overactive gland(s) while preserving the normal functioning glands. This can help restore normal calcium levels in the body and alleviate the symptoms of hyperparathyroidism.
In Conclusion
In conclusion, while the thyroid and parathyroid glands are neighboring structures in the neck and both play essential roles in maintaining overall health, they have distinct functions and impact different aspects of the body’s physiology. The thyroid gland is primarily responsible for regulating metabolism, whereas the parathyroid glands focus on controlling calcium levels in the blood. Understanding these key differences is crucial for diagnosing and managing disorders related to these glands. Both the thyroid and parathyroid glands are vital components of the endocrine system, and their proper functioning is essential for maintaining the body’s equilibrium and overall well-being.

FAQs
The thyroid gland primarily regulates metabolism and body temperature by producing hormones such as T3 and T4.
The parathyroid glands play a crucial role in maintaining blood calcium levels by producing Parathyroid Hormone (PTH).
The thyroid is a single, butterfly-shaped gland, while the parathyroid consists of four small glands, typically found in pairs.
While both glands are located in the neck, the thyroid is situated in the front, just below the Adam’s apple, and the parathyroid glands are found on the posterior surface of the thyroid.
Yes, the thyroid directly influences metabolism, whereas the parathyroid glands do not have a direct effect on metabolism.
Thyroid hormones are regulated by a feedback loop involving the hypothalamus, pituitary gland, and thyroid hormones. Parathyroid hormone production is primarily regulated by blood calcium levels.
Thyroid disorders include hypothyroidism, hyperthyroidism, and goiter. Parathyroid disorders include hyperparathyroidism and hypoparathyroidism, which impact calcium balance.
Yes, thyroidectomy may be required for certain thyroid disorders, and surgery for hyperparathyroidism involves removing overactive parathyroid glands while preserving normal functioning ones.
The thyroid receives blood from the superior and inferior thyroid arteries, whereas the parathyroid glands are supplied by various branches of the thyroid arteries.
Understanding these differences is crucial for accurate diagnosis, treatment, and overall health management, as these glands serve distinct and vital functions in the human body.
Read More:



